With Linda Argote, Carnegie Mellon University and Jeremy M. Kan, University of Pittsburgh
When a trauma patient enters the emergency department, their chance of survival often depends on what happens within the first few minutes after their arrival. After studying trauma resuscitation teams at UPMC Presbyterian in Pittsburgh, Pennsylvania’s largest major trauma center, it’s clear that trauma teams aren’t organized in advance—they’re formed on the fly. Some team members may have worked together many times in the past, while others may be meeting for the first time.
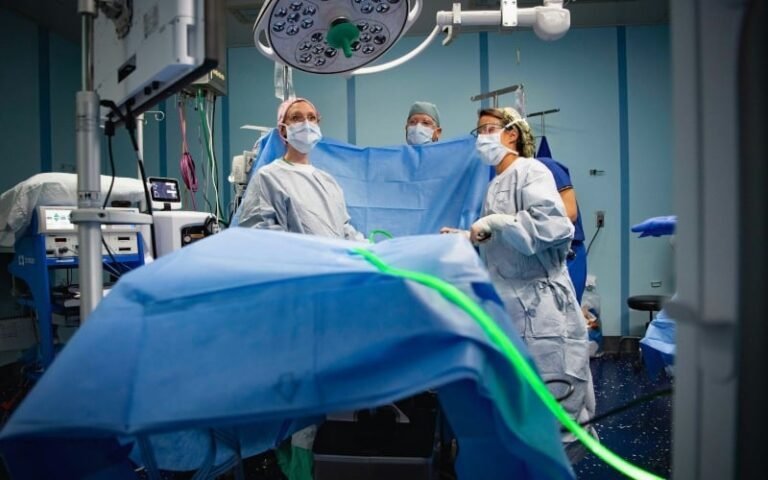
These minutes can be chaotic, fast-paced and high-stakes. The patient is usually wrapped in a stretcher, bleeding, barely breathing and surrounded by alarms and voices. At the bedside are emergency physicians, anesthesiologists, surgeons, nurses and respiratory therapists – a large team of dedicated healthcare providers. Everyone has a job. Everyone moves fast. When it works well, it seems almost effortless. When it doesn’t, small delays can have big consequences.
Medical professionals often say that “teamwork matters” in healthcare. But only a few studies show how Teamwork affects patient outcomes or point to concrete, practical ways to make teams work better together.
This knowledge gap motivated us to come together to study this topic. One of us is one intensive care unit physician and the other is one organizational scientist which studies groups in various settings. We based our approach on a classic idea from behavioral science called interactive memory systems.
Traumatic injuries, such as car accidents, falls, and gunshot injuries, are the leading cause of death for young people around the world. At all ages, Trauma is one of the top killers. Because trauma is widespread, even small adjustments in how emergency teams coordinate can help save lives and shorten recovery times for patients.
Here is where interactive memory systemsTMS, come on. TMS is a shared understanding within a team of who knows what and who is good at what. A team succeeds not because everyone knows everything, but because people rely on each other’s expertise. The team works best when each person knows what they are responsible for, what other team members specialize in, and who to turn to when a specific problem arises.
Team familiarity shapes results
Consider a group of friends playing basketball. The best basketball teams are not the ones that all have the same skills. They are the ones where one person is great at rebounding, one can shoot from long range and another is good at dribbling the ball down the floor. It’s important that everyone knows each other’s skills, so when a specific skill is needed, they know who to turn to.
In trauma care, this kind of knowledge could save lives. When seconds matter, the team needs to know immediately who would be best at placing a breathing tube and who would be best at reading the ultrasound. A strong TMS means fewer questions, less hesitation, and smoother coordination.
For each trauma patient, we measured three things: shared team experience, interactive memory systems, and patient outcomes, based on how long patients stayed in the ICU and in the hospital overall. We were looking for teamwork that showed good coordination, trust in expertise and a clear division of responsibilities.
The Science Behind Who Knows What
Our results were impressive. First, groups with more shared experience had stronger interactive memory systems. The more often people had worked together in the past, the better they seemed to know each other’s skills and coordinate their tasks. If you add up the number of times two team members had worked together in a previous resuscitation and divide by the number of dyads or couples in the team, the average in our study was 10 times. As this number increased, interactive memory systems became more powerful.
Second, stronger interactive memory systems were associated with better patient outcomes. These improvements were substantial: Patients in care groups that were well above average in their interactive memory systems stayed in the hospital about three fewer days and spent nearly two fewer days in the ICU.
Third, TMS explained why shared experience mattered. It wasn’t just that the experienced teams were better, but this shared experience helped the teams create a clearer mental “map” of each other’s expertise. It is this map that has helped patients get better faster.
Trauma care is unpredictable – you can’t always control who is on a team or how often people work together. However, it may be possible to design training procedures and work schedules that help groups build interactive memory more quickly.
More broadly, our study suggests that improving health care is not just about developing new technology or training better doctors. It’s about harnessing the power of teams, helping people quickly understand and trust each other’s strengths when it matters most. For us, one from the bedside and the other from organizational science, this is the exciting next step: turning the science of teamwork into practical tools that help trauma teams save lives.![]()
Linda ArgoteThomas Lord Professor of Organizational Behavior and Theory. Director, Center for Organizational Learning, Innovation and Knowledge, Carnegie Mellon University and Jeremy M. KanProfessor of Critical Care Medicine and Health Policy & Management, University of Pittsburgh
This article is republished from The Conversation with a Creative Commons license. Read it original article.
—
Previously Posted at theconversation.com with Creative Commons license
***
Join The Good Men Project as a Premium member today.
All Premium members can view A full list of benefits is here.
—
Photo source: unscrew
The post Trauma patients recover faster when medical teams know each other well, new study finds appeared first on The Good Men Project.