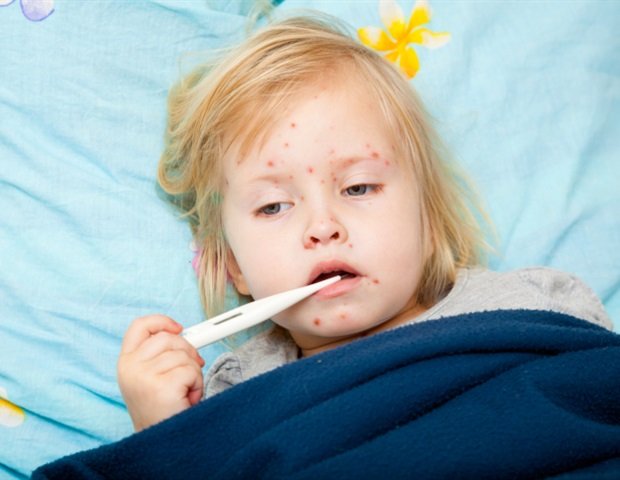
Measles remains one of the most contagious infectious diseases, transmitted through coughing and sneezing, with even small reductions in vaccination coverage leading to outbreaks. As of 2026, California has reported the highest annual number of measles cases in seven years. In response to this growing concern, researchers have begun to examine gaps in knowledge and vaccination coverage about measles.
A UC Riverside study found significant gaps in knowledge, vaccination status, and acceptance of the measles, mumps, and rubella (MMR) vaccine among patients visiting emergency departments in the United States.
Posted on American Journal of Emergency Medicinethe study examines how misinformation and barriers to access may be contributing to lower vaccination rates, raising concerns amid ongoing measles outbreaks.
“We found that a significant proportion of emergency department patients lack accurate knowledge about measles and the MMR vaccine,” said medical student Alexandra Eftimie, lead author of the paper.
Many participants were either unsure of their vaccination status or reported not having received the vaccine at all. In addition, vaccination hesitancy, due to misperceptions of safety and necessity, remains a persistent issue.”
Alexandra Eftimie, UC Riverside School of Medicine
Using survey data (April–December 2024) from 2,459 adult patients in ten US emergency departments, the study assessed MMR vaccination status, knowledge, and willingness to receive the vaccine in a diverse population.
“We found key disparities in undervaccination associated with factors such as race, language, insurance status, and access to primary care,” said Sahithi Malireddy, an undergraduate student in neuroscience and co-lead author of the paper. “These disparities highlighted how systemic barriers shape both vaccine access and health literacy among diverse populations.”
The researchers emphasize that their findings demonstrate how emergency departments can serve as critical “safety net” points of care for underserved populations who may not be able to access vaccines/health care in traditional forms.
“This really offers health care systems an opportunity to leverage emergency departments not only for urgent care, but also as places to deliver accessible, evidence-based public health interventions and improve vaccine equity,” Malireddy said. “By leveraging emergency departments as intervention points, health care systems may be able to reach people who would otherwise fall through the cracks of preventive care.”
The researchers were surprised by how often patients did not have access to clear, reliable information.
“Many gaps stem from systemic barriers such as limited literacy tools, language differences, insurance issues and stigma,” Malireddy said. “They show how culture and access shape responses to symptoms, shifting the focus from individual misunderstanding to structural disparities—and underscoring our responsibility to make health care knowledge accessible and actionable for marginalized communities.”
Senior author Dr. Robert Rodriguez, professor of medicine at the UCR School of Medicine, outlined practical steps emergency departments can take to increase MMR vaccination rates.
“While most emergency departments may not be able to administer MMR vaccines, they can serve as high-impact sites for screening and education — especially for underserved populations,” he said. “They can educate patients about the importance of the MMR vaccine and direct them to accessible options, such as clinics and pharmacies, where they can get it.”
Source:
Journal Reference:
Malireddy, S., et al. (2026). Gaps in knowledge, receipt and acceptance of measles, mumps, rubella vaccines in a national sample of emergency department patients. The American Journal of Emergency Medicine. DOI: 10.1016/j.ajem.2026.03.022. https://www.sciencedirect.com/science/article/abs/pii/S0735675726001452?via%3Dihub.