I think it’s safe to say that if you’re reading this, you want to be healthy. You want to feel strong and energetic and good. You want to reduce your chances of developing a chronic condition. You like getting good news when you get your blood pressure or cholesterol checked. You might be wondering, does weight loss equal health?
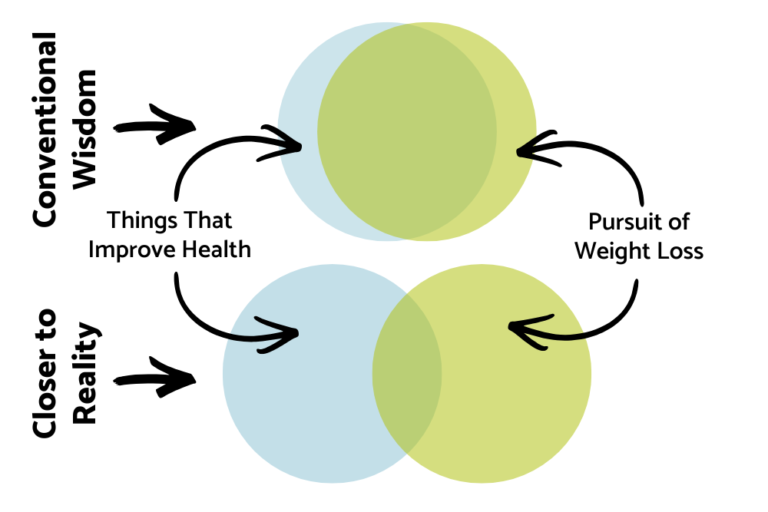
In our society, the dominant idea is this to be healthy, we need to lose weight if we are “overweight” or make sure we don’t gain weight if we are a “normal” weight. Consequently, the conventional wisdom is that pursuing weight loss will also make us healthier in the long run.
(This is sometimes accompanied by the caveat that, of course, some people try to lose weight in unhealthy ways – laxative abuse, purging, extreme diets – but most of the things people do to lose weight that are “healthy”.)
Mmmmm…not so much. in fact, There’s less overlap between “pursuing weight loss” and “pursuing long-term health” than you might think.
Here is a visual representation that is more accurate:
Things that make us healthier (but not necessarily thinner)
There are many, many behaviors that contribute to health, but don’t necessarily contribute to weight loss:
- Regularly participating in enjoyable physical activity long term
- Eating a variety of nutrient and delicious foods
- Eat when you’re hungry and allowing yourself to eat enough to fill you up
- Having access to quality patient-centered healthcare;
- Continuing on preventive health careincluding screenings
- Upbringing meaningful social connections
- Prioritizing getting enough quality sleep
- Managing stress levelsthrough healthy coping mechanisms (this is easier if you also enjoy freedom from oppression and discrimination)
- Cultivating body acceptance
Aspects of diet that can erode our health and well-being
There are also many, many diet-related behaviors that can erode health and wellness:
- Taking one All or nothing approach to exercise (often based on burning calories) which increases the risk of injury and contributes to ‘giving up’ exercise for periods of time
- Limiting amounts and/or types of foods, which can lead to nutrient deficiencies, rebound biging, food obsessionstress, gut health at riskand possibly one eating disorder
- Avoid the doctor because you are unhappy with your weight
- Avoid socializing because “you can’t eat that food” or because you don’t want people to see you at your current weight, resulting in social isolation.
- Waking up in sleep to make time for extra exercise
- Weight cycling (repeated loss and recovery) that over time causes a increase in body fat (known as ‘fat excess’) and a muscle loss
- Pushing your body below a weight range it wants to be in (weight suppression), which leads to a metabolism slowed down

The weight-centered approach to health
Our society and our health care system operate according to a weight-centered approach to health. In other words, the attitude that higher weight = poorer healthand weight loss = improved health. Interestingly, the research doesn’t really support this.
The research is clear that
We need more research to identify the biological mechanisms that explain the second link, but one thing we do know is that stigma and prejudice lead to increased anxiety — including increased levels of the stress hormone cortisol, and ironically can lead to weight gain.
We also know that when stress and elevated cortisol are chronic, as is likely for those with significantly larger bodies (external stigma) and anyone else who feels their body is bad and wrong the way it is (internal stigma), regardless of their body size, it plays a causal role in many health conditions. These include cardiovascular disease, type 2 diabetesand certain cancers.

Flaws in weight loss research
Here’s the problem: very little research on weight and health looks at factors like cardiorespiratory fitness or weight stigma experiences. Suppose some larger-bodied people have worse health:
- Could it be due to the physiological and psychological effects of weight stigma and shame?
- Is it because they don’t exercise, perhaps because they’ve experienced stigma at the gym or rude comments while out for a walk?
If something isn’t measured, we can’t assess it, so if researchers don’t ask about exercise habits/fitness levels and external/internal weight stigma, how do they know if it is really the body weight that is responsible for the ill health?
Another problem is that weight loss research almost never follows participants long enough to find out how many people regained weight and how much weight. They do not consider whether they are still exercising or whether their experiences with weight stigma have increased. They don’t know how to measure the loss of temporary health improvements they experienced while participating in the study.

The approach to health that includes weight
A weight-inclusive approach makes room for all bodies, without dictating that to be healthy, people must change their body size. This approach focuses on adopting habits that are known to benefit health—including the ones I mentioned above—rather than habits that are supposed to change body size or shape.
Although not a weight study, I want to highlight the research from the Diabetes Prevention Program (DPP). This study was designed to promote weight loss, using fat and calorie restriction along with increased physical activity of at least 150 minutes per week. Participants in this lifestyle group were more successful in preventing diabetes than a group taking metformin.
Interestingly, the lifestyle group was much more successful in meeting the physical activity goal than the weight loss goal, but the DPP is usually described as evidence that a small amount of weight loss reduces the risk of diabetes. It might more accurately be described as proof that Regular physical activity reduces the risk of diabetes.
The weight-inclusive approach fully recognizes that not all factors that contribute to health are within our personal control and that the same things that improve the health of a thin person improve the health of a fat person.
These “things” include the many social factors that affect our health. These social determinants of health they include the conditions in which we live, work, and play, and those conditions include our access to health care and whether we experience bias, stigma, and discrimination based on weight, race, gender, or other aspects of ourselves.
Making the mental shift
Naturally, Moving to a mindset that includes weight on a personal level requires a fair amount of “unlearning.” In other words, getting over the idea that weight = health, and also getting over the idea that weight = our value as a human being.
Let’s face it, even when we pursue weight loss in the name of “improved health,” there’s that part of us that seeks society’s approval by achieving—or at least approaching—the slim ideal. In fact, a consumer survey by the International Food Information Council found that appearance ranks above health as reasons for starting a diet.
The most important health behaviors are those that support both physical and psychological well-being. We want to keep doing them no matter what size we are, and they make our lives bigger and better, not smaller and more stressful.
Having a healthy relationship with food and an effective self-care routine doesn’t require obsession and rigidity, and it doesn’t lead to anxiety and self-righteousness when things don’t go according to plan. It’s a journey, not a test. There is no success, only learning and curiosity and evolution.

Disclaimer: All information provided here is general in nature and provided for educational purposes only. This information should not be taken as medical or other health advice related to an individual’s specific health or medical condition. You agree that use of this information is at your own risk.
Hi, I’m Carrie Dennett, MPH, RDN, a weight that includes registered dietitian, nutritionist and body image consultant. I offer compassionate, personalized care to adolescent adults of all ages, shapes, sizes and genders who want to heal eating disorder, disordered eating or years of dietingthey cultivate an accepting, respectful relationship with their bodies and gain the freedom to live an authentic, meaningful life without obsessing over food.
Need 1-on-1 help with your nutrition, food or body image concerns? Schedule a free 20-minute Discovery Call let’s talk about how I can help you and explore if we’re a good fit! I am in network with Regence BCBS, FirstChoice Health, Providence of Oregon Health Plan and United Healthcare and can bill Blue Cross and/or Blue Shield insurance in many states. If I don’t get your insurance, I can help you claim compensation yourself. To learn more, explore our insurance and service areas page.
![]() Print this post
Print this post